Pulmonary Stenosis
What is it?
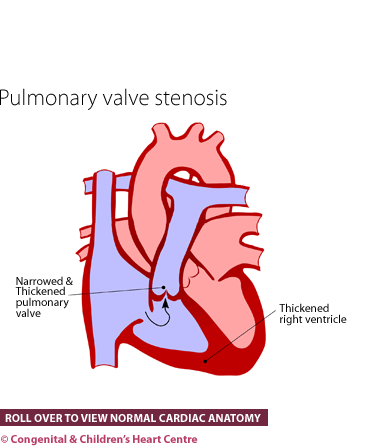
Pulmonary stenosis (or PS) is a condition whereby the amount of blood going to the lungs is limited because of narrowing of the pulmonary artery, either at the valve or just below or above it. In the type that affects the valve itself, the three parts of the valve (valve leaflets) can be abnormal, leaving them sometimes too thick or sometimes fused together.
The effects of this narrowing are that the heart muscle has to work harder to pump the blood to the lungs. The heart muscle becomes much thicker in the relevant pumping chamber, the right ventricle. This can potentially reverse itself if the narrowing is removed.
How many people get it?
The prevalence of pulmonary stenosis has been estimated at 8 cases per 10,000 live births and this accounts for about 8% of all congenital heart disease.
Who gets it?
Anyone can get pulmonary stenosis. It may be present at birth or even in the womb. It is not a static problem and it can sometimes be seen to progress over the last 12 weeks of pregnancy. It can occur in children with a condition called Noonan syndrome. These children have a characteristic facial appearance and may also have a problem with the heart muscle itself.
What are the signs and symptoms?
Pulmonary stenosis is often present without there being any symptoms at all. The condition may be detected as a murmur (a noise heard when listening to the heart with a stethoscope) at a routine health screening or during a medical examination for other reasons. It can sometimes be found in children with Noonan syndrome who are under investigation. When it is severe, it may cause tiredness on exertion, breathlessness on exercise or even fainting.
There is a type that occurs in newborns and that is called critical pulmonary stenosis. This is when there is such severe narrowing of the pulmonary arteries that, after birth, little blood gets to the lungs. The baby usually becomes blue on the lips and tongue on the first or second day of life and may then become very unwell before treatment is started.
With the advent of fetal echocardiography (ultrasound scanning of the unborn child's heart), the diagnosis can sometimes be made before the child is born. This allows arrangements to be made for the infant to be seen in a cardiac centre after birth.
What kind of tests might I have?
Infants are usually referred to a paediatric cardiologist, who will investigate further. After questioning the parents to obtain the child's history and examining the child, several tests will be organised.
These will usually consist of an electrocardiogram (ECG) to measure the electrical activity of the heart and a chest X-ray to visualise the heart and lungs. The diagnosis is made by echocardiography. This ultrasound scan will show that the artery to the lungs is narrowed at some point. Some blood tests may also be necessary.
What is the treatment?
Treatment is only needed when the narrowing is of a sufficient severity to be a concern. Some people with only mild or moderate narrowing never need any treatment.
- Drug treatment in newborns with severe valve narrowing (known as critical pulmonary stenosis). A drug called prostaglandin is administered to keep open a pipe (the duct) that is open in the womb but that usually shuts after birth. This allows blood to enter the lungs until a more permanent treatment can be given (usually ballooning).
- Balloon valvuloplasty at cardiac catheterization. If treatment is needed and the narrowing is at the level of the valve then the valve can be directly ballooned internally. Essentially a catheter is inserted through the leg vein under general anaesthesia and a balloon placed across the valve. When inflated the valve stretches up. The catheter and balloon are then removed.
- Surgery. When the narrowing is below or above the valve and severe enough to require treatment, surgery is necessary.
What is the prognosis?
The prognosis for this condition is generally good, with survival without complications nearly 100%. In the long term, these children fare well and most have no symptoms and lead normal lives. Some children require repeat balloon procedures. Sometimes the narrowed valve becomes leaky after an operation and this itself can be a problem ultimately needing surgical replacement in later childhood or early adulthood.
Download Pulmonary Stenosis PDF![]()
Further information at The Children's Heart Federation

