Tetralogy of Fallot
What is it?
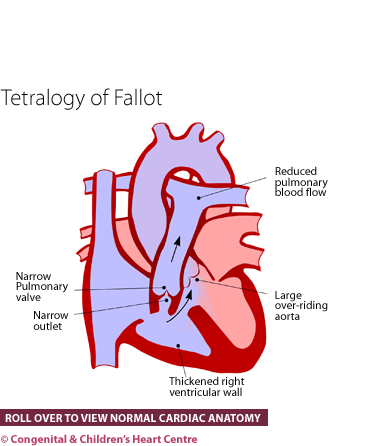
Patients with Tetralogy of Fallot have 4 abnormalities (hence tetralogy):
- Pulmonary stenosis
- Ventricular septal defect
- Overriding aorta
- Increased musculature of the right ventricle termed hypertrophy.
Pulmonary stenosis (PS) is narrowing in the outflow from the heart that leads to the lungs, and this can be at, below or above the valve. A ventricular septal defect (VSD) is a hole between the main two pumping chambers of the heart – the right and left ventricles. When the narrowing is severe, blood in the right ventricle will pass across this VSD and go straight to the aorta, which is the main blood vessel to the body. This causes blue blood returning from the body to return back to the body without visiting the lungs first to pick up oxygen. The infant or child will then appear blue on the lips and tongue. As a consequence of the narrowing of the outflow to the lungs, the relevant pumping chamber (right ventricle) often develops severe muscular thickening because it is working harder than normal (hypertrophy).
An overriding aorta means that the main blood vessel to the body (aorta) sits directly over the hole in the heart rather than coming from the left ventricle only.
How many people get it?
There are about 5 cases of Tetralogy of Fallot out of every 10,000 live births accounting for about 5% of all congenital heart disease.
Who gets it?
Anyone can get Fallot's but it is commoner in certain conditions, such as DiGeorge syndrome (22q11 deletion). It can be inherited and so run in families.
Whatever the cause of Fallot's tetralogy, it is present from birth and, in fact, from very early on in the pregnancy (possibly the 7th week after conception).
What are the signs and symptoms?
Tetralogy of Fallot usually comes to medical attention in infancy with cyanosis or blueness, although it may be detected at health screening checks as a murmur (abnormal heart sound). Cyanosis (blueness) occurs when the dominant feature is pulmonary stenosis (narrowing of the blood vessel to the lungs). The blueness will be obvious on the lips and tongue.
If the blueness is around the lips, or on the face, hands or feet but not the tongue, then this is more likely to be due to reduced skin circulation and is not caused by tetralogy of Fallot.
Some infants visit their doctor at a few months of age with severe blue episodes termed spelling. After crying or emotion, they become severely blue and irritable, often drawing their knees up to their chests. Sometimes, they may lose consciousness. After a few minutes, they usually recover. Older children may squat on their haunches during an attack. Features such as these are very serious and immediate medical attention should be sought. Drawing the knees to the chest or squatting are nature's way of helping an attack and should not be prevented.
If the pulmonary stenosis (narrowing) is mild, the infant may go to their doctor with breathlessness, a murmur and a normal pink colour. However, these children may also go on to have blue or cyanotic spells.
With the advent of fetal echocardiography (ultrasound scanning of the unborn child's heart), the diagnosis can sometimes be made before the child is born. This allows arrangements to be made for the infant's transfer to a cardiac centre after birth.
What kind of tests might I have?
Infants with Tetralogy of Fallot are usually referred to a paediatric cardiologist, who will investigate further. After questioning the parents to obtain the baby's history and examining the child, several tests will be organised.
These will usually consist of an electrocardiogram (ECG) to measure the electrical activity of the heart and a chest X-ray to visualise the heart and lungs. The diagnosis is made by echocardiography.
Prior to surgery, cardiac catheterisation may be required to give the surgeon additional information.
What is the treatment?
- Drug treatment. Initially, the infant may not need any treatment and can merely be observed. If the child becomes very blue or develops spelling episodes, then a type of medicine called beta-blockers may be started (examples include propranolol or atenolol).
- Balloon valvuloplasty at cardiac catheterisation. The narrowed pulmonary valve is stretched internally using a cardiac catheter inserted into the leg vein. This is a temporising measure that may be required in certain circumstances.
- Surgical treatment. The age at which this is performed and the surgical strategy may vary.
- Shunt procedure (for example a modified Blalock-Taussig shunt) may be performed first if the infant is very blue or having blue episodes. A shunt is an artificial pipe into the lung arteries that delivers extra blood to the lungs and reduces the blueness by making the child pinker.
- Complete repair is performed when the child is about 6 to 12 months of age. This requires open-heart surgery and the use of cardiopulmonary bypass. The hole (VSD) is closed and narrowing of the valve (PS) repaired. Once this has been performed, the thickening of the muscle spontaneously regresses.
In some cases, the total correction is performed as the only procedure. There are risks and benefits of both strategies.
What is the prognosis?
The prognosis for this condition is generally excellent. In the long term, these children fare well and most have no symptoms. In some cases the narrowed valve becomes leaky after the repair. These patients may have reduced exercise tolerance in later childhood and may require a further operation to replace the pulmonary valve. There is a low occurrence of heart rhythm problems in the longer term.
Download Tetralogy of Fallot PDF![]()
Further information at The Children's Heart Federation

