Ventricular Septal Defect
What is it?
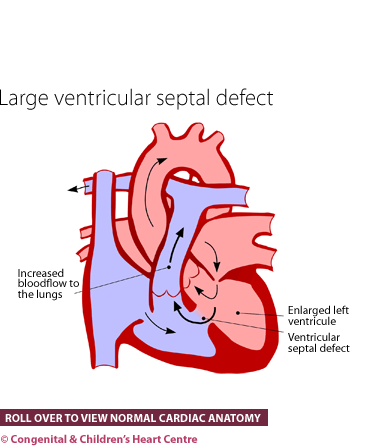
Ventricular septal defect (VSD) is a condition whereby there is a hole between the two pumping chambers of the heart. The defect can be small or large. The VSD may be termed muscular, perimembranous, inlet, outlet, apical or doubly-committed depending on its position and the surrounding substance of the heart.
Where the VSD is small, there is no elevation of the low pressures found in the right ventricle (pumping chamber to the lungs) and therefore the lungs are also low pressure (as they should be). Where the hole is large, the pressure in this right ventricle can be elevated; sometimes equal to that of the high pressure left ventricle (pumping chamber to the body).
There may be more than one defect in any patient and they can occur with other types of congenital heart disease.
How many people get it?
It has been estimated that there are 3 cases of VSD out of every 1,000 live births accounting for about one third of all congenital heart disease.
Who gets it?
Anyone can have a ventricular septal defect. Whatever its cause, it is present from birth and probably from very early on in the pregnancy (possibly the 7th week after conception).
What are the signs and symptoms?
Small defects often cause no symptoms but come to medical attention as a murmur on a routine health screening, often at the discharge baby check or the 6 week check.
Infants with medium-sized defects may come to medical attention with breathlessness particularly on feeding. This is known as heart failure and may limit the amount of feed the baby takes. The extra effort that the heart has to make, can lead to poor weight gain. The baby may also sweat during a feed and this can be seen on the infant's forehead. He or she may be prone to chest infections. If the child manages to grow, the hole may become relatively smaller and the effects may lessen and eventually disappear. In childhood, the child may have slightly less energy than his or her peers.
Large defects will usually come to medical attention in the first couple of weeks. The symptoms are of severe breathlessness, often at rest, and poor feeding, with sweating. There may be chest infections as well. The baby may retain fluid. These symptoms and signs may persist despite treatment. Surgical closure of the defect is usually necessary in these cases.
With the advent of fetal echocardiography (ultrasound scanning of the unborn child's heart), the diagnosis can sometimes be made before the child is born. Referral can then be made to a paediatric cardiologist prenatally.
What kind of tests might I have?
Infants are usually referred to a paediatric cardiologist, who will investigate further. After questioning the parents to obtain the child's history and examining the child, several tests will be organised.
These will usually consist of an electrocardiogram (ECG) to measure the electrical activity of the heart and a chest X-ray to visualise the heart and lungs.
The diagnosis is made by echocardiography. This ultrasound scan will show the hole or holes in the heart and can measure the speed and direction of blood crossing the hole. This uses a special function on the echo machine called colour Doppler. Some blood tests may also be necessary.
What is the treatment?
Treatment depends on the size of the hole and its effect on the heart.
- Observation only. Small defects rarely cause a problem and are usually only monitored.
- Drug therapy. Medium-sized defects may need treatment when breathlessness and heart failure ensue. This would initially be with medicines called diuretics such as frusemide and spironolactone. Diuretics cause the infant to pass more urine and thus reduce the amount of fluid that can accumulate on the lungs, making breathing and feeding easier. Another type of medicine called an ACE inhibitor, such as captopril, can be used. Sometimes, calorie supplements need to be added to the feed to increase the baby's growth.
- Surgery
- Complete repair. Large defects will be treated with the same medicines and calorie supplementation but will need surgical intervention.
- Staged repair. If there are multiple holes that would require difficult surgery to close them off (for example, if they are at the very bottom of the heart), a staging procedure may be needed. This would involve banding of the artery to the lungs (pulmonary artery banding) to prevent high pressure and, hence, damage to the lungs. At one to two years of age, this operation would be reversed and the holes closed. It would then be easier as the child would be bigger. Cardiac catheterisatio0n may be needed prior to surgery.
Rarely, moderate-sized defects can be closed by cardiac catheterisation). An umbrella or plug type of device is deployed internally positioned to close the hole.
What is the prognosis?
Children with small holes will lead normal lives with no limitation at all. Sometimes they will close off completely by themselves. Even if they do not, they are highly unlikely to lead to any harm. Children who have had larger holes closed at surgery have an excellent prognosis and in the long term fare well without symptoms leading normal lives.
Children presenting after about 12 months of age, and sometimes younger, may develop irreversible lung damage. Blood may flow across the hole the other way avoiding the lungs, causing the child to become blue. This is termed Eisenmenger syndrome. Such children will develop breathlessness and reduced exercise tolerance and have reduced longevity. In the current era this is extremely rare.
Download Ventricular Septal Defect PDF![]()
Further information at The Children's Heart Federation

